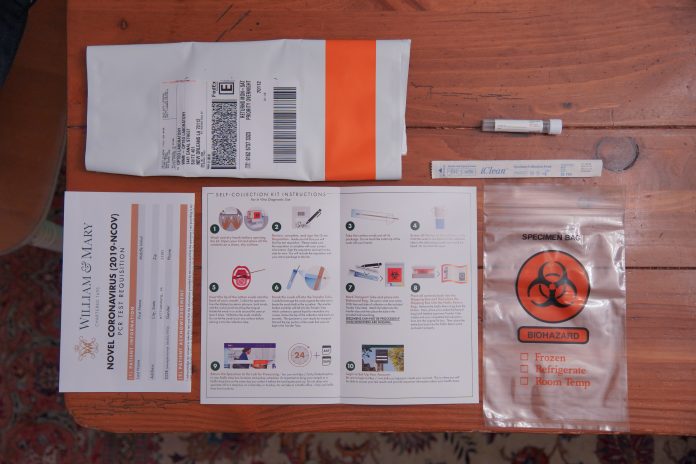
As the College of William and Mary reopens this fall, pre-arrival and on-campus prevalence testing has been an integral part of the College’s path forward. Last week, The Flat Hat reported that Kallaco, the company contracted to administer the pre-arrival testing, has relied on testing that has not been granted Emergency Use Authorization by the U.S. Food and Drug Association.
The tests, which were conducted at New Orleans based Opteo Laboratories, are categorized as Laboratory-Developed Tests — tests that have been designed for manufacturing and use in a single laboratory. Who is responsible for the regulation of LDTs has been in question since before the COVID-19 pandemic, yet the need for accurate and fast COVID-19 testing has rekindled the debate.
Aug. 21, the Trump administration rolled back the FDA’s ability to regulate LDTs. This new policy allows laboratories to distribute tests without the FDA’s review. The FDA has come under fire in the past for the arbitrary enforcement of its LDT regulations. Some health experts applaud the removal of red tape to increase the number of COVID-19 tests available while others have expressed concerns over the accuracy of tests that have not undergone pre-market approval by the FDA.
“The science behind it is that we don’t have enough assays and it’s taking time to get them to market. We’re having trouble scaling up innovation. Arguably we’ve had six months to do that and we still haven’t been able to scale up.”
“There are reasons why they relaxed the rules that have to do more with politics than science,” Research Associate at Johns Hopkins University Paul Stamper said. “The science behind it is that we don’t have enough assays and it’s taking time to get them to market. We’re having trouble scaling up innovation. Arguably we’ve had six months to do that and we still haven’t been able to scale up.”
With over 4,000 students being tested before the Trump administration’s Aug. 21 announcement, the College has found itself in the middle of a decades-long debate within the scientific community. After it was revealed that students were indeed tested with an LDT that had not been granted EUA, the College announced in a Sept. 7 email that all students living on campus will be required to undergo another round of testing which will be performed by Wisconsin Diagnostic Laboratories, in partnership with VCU Health. The new tests will be collected by medical professionals in Kaplan arena.
Wisconsin Diagnostic Laboratories says it uses a Center for Disease Control developed PCR assay test, which has been granted EUA by the FDA. The Flat Hat confirmed that the laboratory is accredited under the Clinical Laboratory Improvement Amendments of 1988.
The College still maintains that Opteo was authorized to distribute its LDT as a laboratory accredited through the CLIA .
“But we have changed labs until we have a clearer answer to Opteo’s authorizations.”
“As a CLIA-certified lab, Opteo’s testing procedures must be rigorously validated well beyond the rapid-turnaround FDA approval process under COVID-19,” the College said in a Sept. 4 statement. “But we have changed labs until we have a clearer answer to Opteo’s authorizations.”
While the recent change in regulation does allow Opteo to distribute its test without FDA authorization, CLIA accreditation and EUA are not equivalent. CLIA does require high standards for its labs, but it does not focus specifically on device efficacy.
Though Opteo notified the FDA of its LDT, the request remained submitted, but not reviewed, according to Kallaco spokeswoman Amy Cheronis. The FDA would not comment on the status of Opteo’s submission.
If Opteo’s submission stalled, Stamper said that might indicate a problem with the test, since the FDA has a finite amount of time to respond to a proposal.
“That means it didn’t meet their minimum requirement to remain a test that is emergency use authorized and move on to the next step for getting to be an FDA approved assay,” Stamper said. “So yeah, they should be worried. Something was wrong with the proposal that was submitted with the performance of the assay or the performance of the laboratory. You don’t know unless you actually saw that report.”
The test’s pending status could indicate that the data is not sufficient enough to prove its accuracy, according to Stamper. Students reported a label on the test collection tubes indicating that it was not intended for diagnostic purposes. Though Cheronis said this label referred to the tube alone, which is not a diagnostic element of the kit, the label could actually be indicative of a larger problem.
“The reason you would be concerned if it’s for diagnostic use only is the quality of the validations,” Stamper said. “If it’s for research use only, typically they’re still in the process of getting the data.”
Opteo did not respond to The Flat Hat’s request for comment.
The confusion over Kallaco has left many students wondering how much the College knew about Opteo’s authorization status and whether they should have done more research before using Kallaco to administer testing.
Cheronis said that Kallaco provided the College with the specifications of the test and the acknowledgment of the FDA’s receipt of Opteo’s submission, though she indicated the College was not made aware of the test’s status as an LDT.
“Under the FDA/EUA process the Opteo Laboratory test was “authorized” as defined by the EUA guidelines.”
“Kallaco was not required to disclose this level of detail to clients but was required to confirm the testing being done was authorized by the FDA, which was part of our contractual obligation,” Cheronis said in an email. “Under the FDA/EUA process the Opteo Laboratory test was “authorized” as defined by the EUA guidelines.”
Cheronis maintained that Opteo was allowed to test while it was waiting for a decision on its EUA submission, which is still pending. College spokeswoman Suzanne Clavet did not comment on the College’s decision to use a test that was pending EUA.
The College also argued that Opteo’s LDT is suitable for home collection of specimens — that is, the test is effective with a throat swab collected by students themselves.
“Like many certified clinical testing laboratories in the United States that conduct COVID-19 tests, Opteo is allowed to use both self-collected and clinically-collected samples for diagnosis under the same EUA,” Chief Operating Officer Amy Sebring said in an Aug. 26 email to students, faculty, and staff.
According to the latest guidelines from the Centers for Medicare and Medicaid Services, which oversees CLIA accreditation, home specimen collection is not permitted unless explicitly authorized under EUA, even for LDTs.
A spokesperson for the FDA confirmed that Opteo’s LDT has never been on a list of LDTs for COVID-19. Furthermore, there are currently 23 tests authorized for home collection through nasal swabs or saliva samples. No tests have been authorized for home collection via oropharyngeal (throat) swab, which is the method students were instructed to collect their samples.
Stamper emphasized the importance of good science and data-driven solutions to a lack of adequate testing capacity in the United States. Though he said companies such as Kallaco may not be at fault, he emphasized the need for transparency.
“We have a great need and we certainly have too few people who can do the testing and too few assays,” Stamper said. “Relaxing the rules and the stringency of those is probably not the way to do it. I think there has to be transparency and oversight.”
Thus far, 20 students have tested positive in the first round of pre-arrival testing. No students and fewer than 10 faculty have tested positive in the on-campus prevalence testing. Still, accurate testing is vital to making informed public health decisions.
“I think the fear for a lot of clinical scientists is that things are being relaxed too quickly. We know the need is great, but these are people’s lives at risk.”
“I think the fear for a lot of clinical scientists is that things are being relaxed too quickly,” Stamper said. “We know the need is great, but these are people’s lives at risk.”
